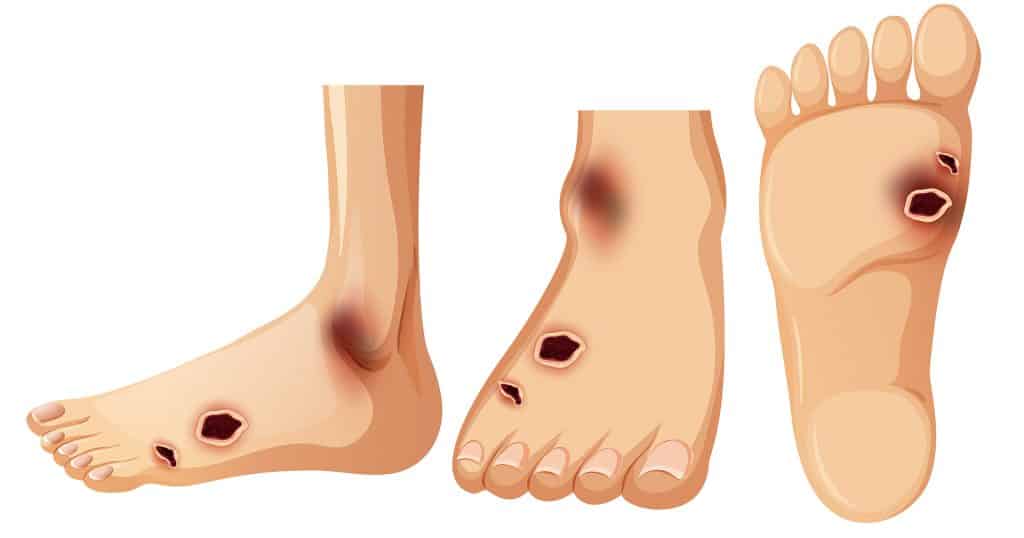
Diabetes can affect your feet in a number of ways. It can cause damage to the nerves that give feeling or sensation to your feet but also circulation.
Why is it important to look after your feet, especially if you have diabetes?
Diabetes can affect your feet in a number of ways. It can cause damage to the nerves that give feeling or sensation to your feet but it can also cause damage to the blood supply or circulation in your feet.
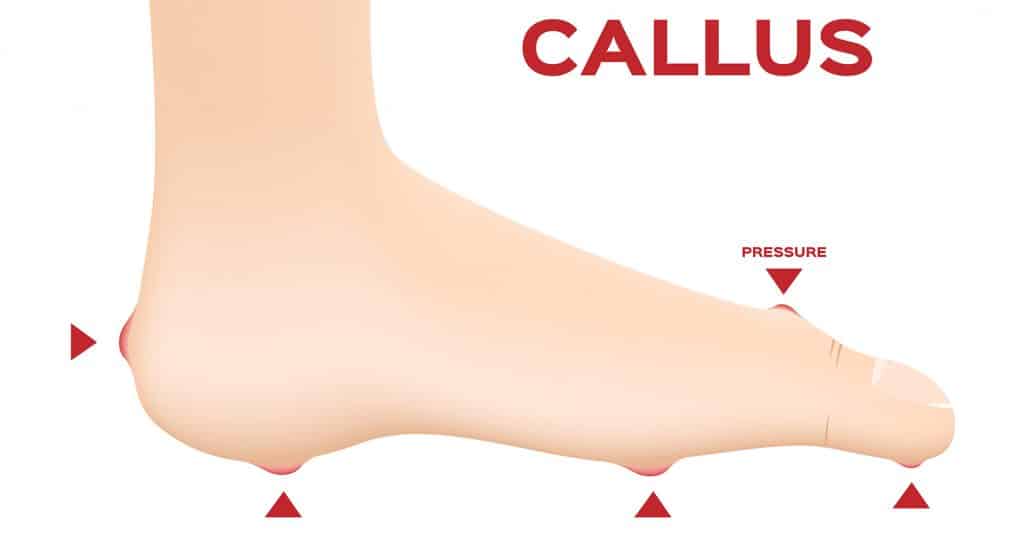
Some of the common signs or symptoms of nerve damage in the feet might be a feeling of numbness, pins or needles, tingling or burning but It is very important to note that many people with nerve damage in their feet from diabetes, have no symptoms or signs at all. The loss of feeling in the feet can result in undetected, painless injuries that may progress to become infected before they are even noticed. Simple injuries or lesions like blisters, cracked skin or even callus can form diabetic foot ulcers. If there is poor circulation then foot ulcers can become very difficult to heal and in some cases this can lead to amputations.
How often do you have to have your feet checked by a Podiatrist?
If you have just been diagnosed with diabetes, it’s a good time to visit your podiatrist for a diabetic foot checkup – the foot checkup screens for nerve damage (or neuropathy), balance, circulation problems, foot deformities and associated skin lesions like callus or corns and a footwear assessment is usually completed.
The diabetic foot checkup helps us to categorise each patient as having low risk, intermediate risk or high risk of developing diabetic foot disease.
Low risk feet are those people with normal sensation and good circulation in their feet. These people need to see their Podiatrist Samford every year for a diabetic foot checkup to detect any changes early.
People with high-risk feet have nerve damage and have had a foot ulcer or amputation in the past. These people should be seeing their podiatrist more frequently to keep their feet safe, at least every 3 months or more regularly.
Why are undetected foot problems dangerous?
Most people with a foot injury seek medical care because of pain, but for people with diabetes, foot problems can go undetected because nerve damage makes foot injuries painless, so these people often don’t seek help until much later, by which time the wound has become much larger, or infected or deeper, affecting the underlying bone, placing them at risk of amputation.
About 15% of people with diabetes will develop a foot ulcer in their lifetime and once you have had a foot ulcer you are 36 times more likely to develop another foot ulcer in the future.
Australia has the 2nd highest rate of diabetes-related amputations in the developed world, so this is a big problem here. However, It is important to emphasise that these diabetic foot ulcers and amputations are preventable and Podiatrists work very hard to prevent foot problems from developing into ulcerations and we play an important role in amputation prevention.
Is there some sort of special footwear needed if you have Diabetes?
If you have low risk feet (healthy nerve supply, good blood circulation) there are no special footwear requirements, we simply recommend that you wear shoes that protect your feet, that fit your feet well and are appropriate for the activity that you use them for.
On the other hand, if you have high risk diabetic feet with nerve damage and perhaps a foot ulcer, then we are likely to recommend special types of medical grade footwear that will help to protect your feet, help the ulcer to heal and prevent future foot problems.
We recommend to all of our patients with diabetes to avoid barefoot walking to prevent injuries to their feet. When buying shoes, you should always try to have your shoes professionally fitted so you know that the fit is correct.
If you notice any changes with your feet what action should you take?
Get into the habit of checking your feet for injuries every day. Look for any cuts, sores, blisters, splinters, redness or swelling.
If you notice an injury, clean the area and apply an antiseptic (like betadine solution) and cover with a sterile dressing and make sure you see your Podiatrist or doctor as soon as possible to ensure the wound heals quickly and that any infection is treated early, early intervention is so important in preventing serious complications and keeping your feet safe.
Some very simple advice for keeping your feet safe:
- Keep your blood sugar levels well controlled – work hard with your doctor or diabete educator to keep your BSLs within normal range;
- check your feet every day for problems and seek help early;
- wear well -fitting protective shoes
See your Podiatrist for regular diabetic foot checkups to prevent problems from occurring.