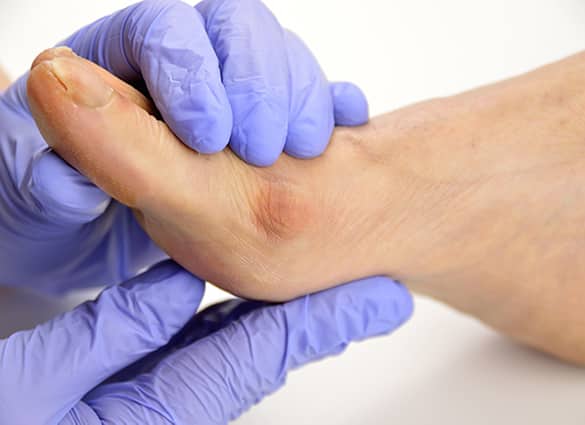
Bunions
Common deformity
A bunion (or hallux valgus) is a very common deformity of the big toe joint, affecting approximately 25% of adults. A bunion is when your big toe (hallux) becomes angled toward the second toe, causing a bony prominence or ‘bump’ at the base of the big toe. Bunions are a progressive foot problem, leading to the development of early osteoarthritis and foot pain, difficulty fitting footwear and unsightly foot and toe deformity.
A bunion may develop in one or both feet and affect females more commonly than males. Certain factors, such as shoe style, types of activity and heredity may affect the severity and rate of development of bunions.
What causes bunions?
A bunion forms when there is a disruption to the normal balance of forces exerted across the big toe joint. This can lead to biomechanical instability in the foot, causing excessive strain across the big toe joint.
Biomechanical instability in the foot can be caused from:
- flat feet
- excessively pronated feet (rolling in)
- joint hypermobility
- weak foot muscles
- a short first metatarsal bone
Although bunions tend to run in families, it is the foot type that is passed down – not the bunion. Parents who suffer from poor foot mechanics can pass their problematic foot type on to their children, who, in turn, are also prone to developing bunions.
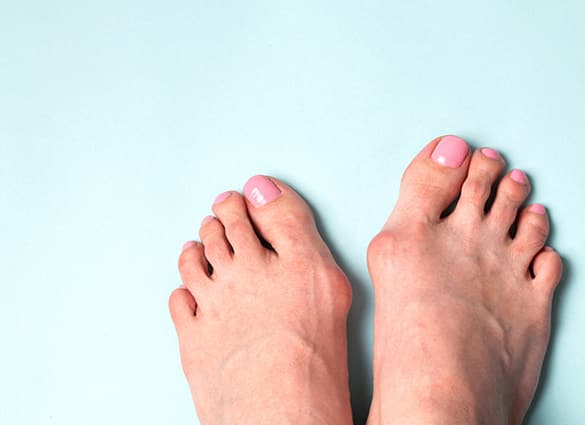
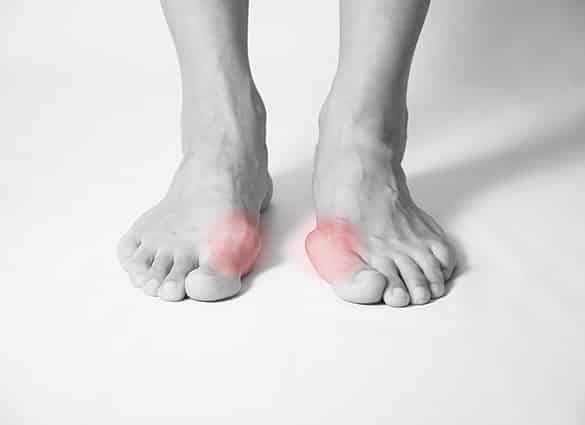
Other causes of bunions
Other causes of bunions include:
- Footwear – wearing shoes that have high heels, or are too narrow, cause the toes to be squeezed together into an unnatural position. This is a common aggravating factor and may explain the high prevalence of bunions among women
- Trauma – fractures, sprains, nerve injuries
- Rheumatoid arthritis or gout
- Occupations that place increased stress on the feet (e.g. ballet)
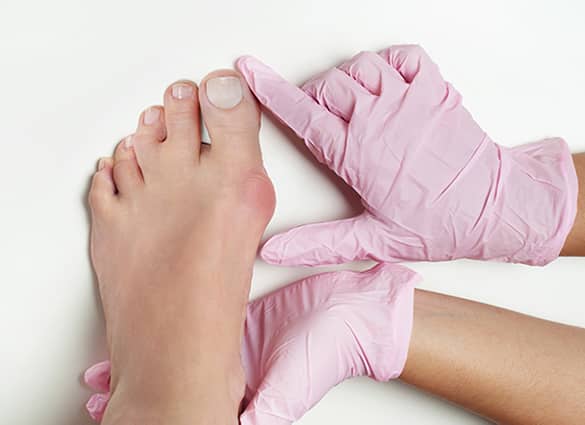
What are the symptoms of bunions?
In the early stages, bunions may be completely asymptomatic. As bunion deformity progresses, you might complain of:
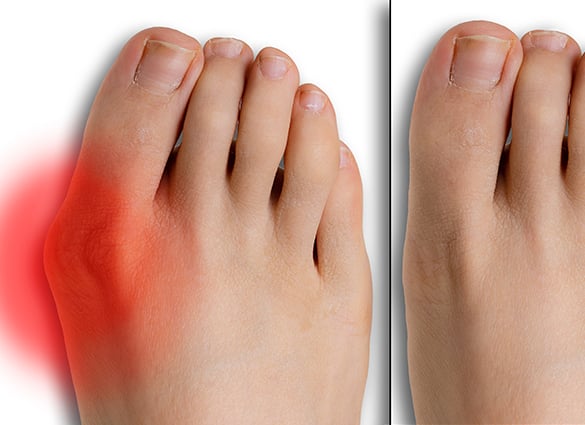
- A bony bump at the base of the big toe joint
- Swelling, or sometimes, redness at the base of the big toe
- Pain beneath the forefoot when walking or exercising (metatarsalgia)
- Deep, aching pain at the bunion joint
- Deformity of the 2nd toe (hammer toes)
- Difficulties finding shoes to fit comfortably
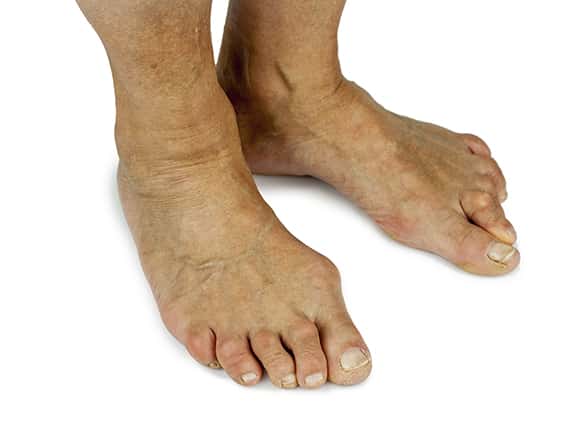
How are bunions diagnosed?
Your Podiatrist will take a comprehensive medical history and perform a physical examination and gait analysis. The assessment will include:
- Foot posture assessment
- Joint range of motion (flexibility)
- Foot muscle strength testing – looking for any muscle imbalance or weakness
- Biomechanical assessment of the foot, ankle and leg
- Footwear assessment
- Gait analysis – to look for any abnormalities in the way the feet move during gait
A plain xray may also be ordered to look more closely at the alignment of the big toe joint and for signs of osteoarthritis.
Do bunions need surgery?
If your bunion is severe and progressive and continues to cause pain even with conservative podiatric treatment, surgery may be the best treatment option.
Several surgical procedures are available to correct bunions. The surgery will remove the bony enlargement and restore the alignment of the toe joint. Bunion surgery is usually a day surgery or an overnight procedure. Recovery takes some months and swelling and discomfort may be present up to 6 months after the procedure.
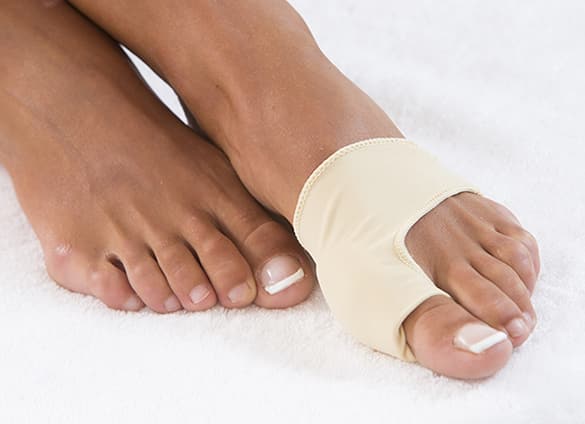
It is important to note that even after bunion surgery, you will be advised to wear low-heeled shoes with a wide toe box and will often need to use foot orthotics to achieve best results.
What should I do if I have bunions?
Bunions are progressive, and may be visible for many years before they become painful. If allowed to progress, however, they can lead to arthritis developing within the joint, causing it to become stiff and painful and shoes will be difficult to fit.
It is important to seek treatment early for bunions because once they progress past the threshold for early treatment options you may need surgery to repair the toe joint.
You should see your podiatrist as soon as possible if you suspect you have bunions. If you think you have a bunion, or you have a family history of bunions, contact us.