Common health problem
Fungal infection of the toenail (or oncyhomycosis) is a common foot health problem, causing embarrassing unsightly, thickened, discoloured nails. Toenail fungus is the most common nail disease in adults, affecting up to 10% of the population.
What causes a fungal toenail infection?
Fungal toenail infections occur when microscopic fungi enter the nail, spreading into the nail plate and the surrounding skin, through the warm and moist environment in socks and shoes.
The toenails are especially vulnerable around damp areas where people are likely to be walking barefoot such as swimming pools, change rooms and communal showers. Some people seem to be more susceptible to developing fungal nail infections. These may include the elderly, people with diabetes, circulation problems and immune-deficiency conditions.
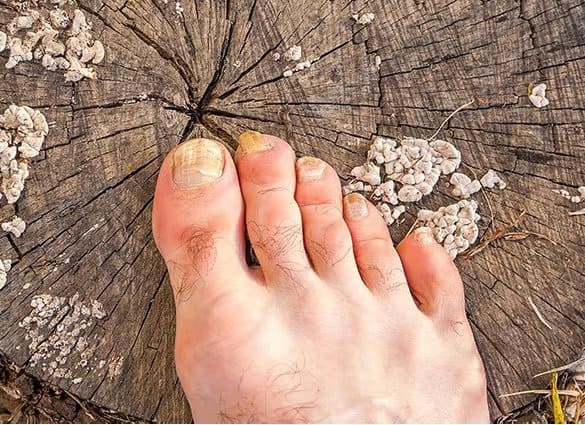
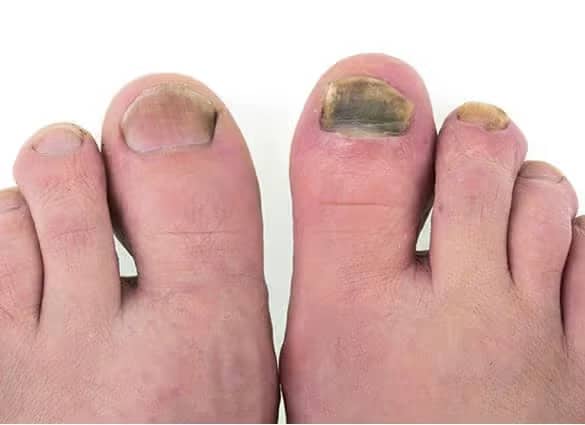
How do I know if I have a Fungal Toenail Infection?
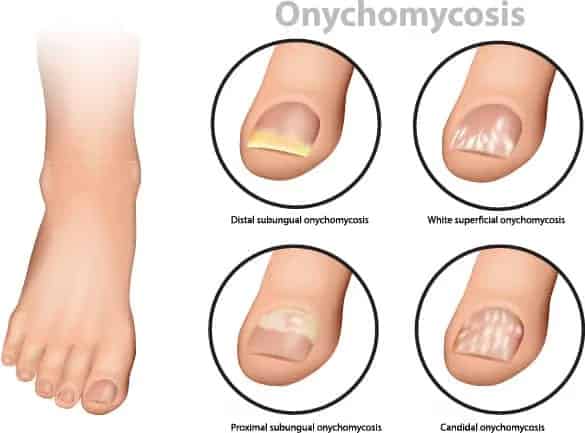
If you have a fungal nail infection you may notice that the toenail has become thickened, yellowish-brown or milky-white in colour, and sometimes malodorous. A build up of nail and skin may collect beneath the nail plate, and the nail may detach from the skin under the nail.
The infection is capable of spreading to your other toenails, the surrounding skin, and even the fingernails and to other members of your household. Fungal nail infections aren’t usually painful, however, if they cause excessive thickening of the nail plate this can result in some tenderness when wearing enclosed shoes and difficulties trimming the nail.
To establish or confirm the diagnosis of a fungal toenail your Podiatrist or doctor may decide to send a sample of the affected nail for a lab test.
How are fungal toenails treated?
Nail infections don’t get better without treatment, and may get worse, affecting more of the nails and surrounding skin. The earlier treatment is commenced, the easier it is to treat.
Until recently, fungal toenail infections were treated with antifungal nail lacquers or oral medications. Antifungal toenail lacquers have not proven to be very effective and patients have experienced poor success rates and high recurrence rates. With oral medications there is the risk of side effects such as liver toxicity and this is generally not a preferred option for most people.
Fortunately, medical technology has introduced a revolutionary method of treating fungal nail infection that’s not only effective, but is 100% safe with no side effects. The Erchonia LUNULA Laser is a low-level laser device bringing new hope to people suffering from thickened, discoloured and unsightly toenails associated with nail fungus. It uses low-level laser light to stimulate the growth of strong, clear and healthy nails.
For best results, the Erchonia LUNULA Laser is used in combination with debridement of the affected nail(s) by your Podiatrist to remove diseased nail matter and debris. The number of treatments required to restore clear, healthy nails will depend on the severity of your nail infection. Remember, the earlier treatment is commenced, the easier it is to treat.
Here are some reasons that make Erchonia LUNULA Laser an increasingly popular choice to treat unsightly fungal toenail infections:
- A high success rate of approximately 80%
- No side effects
- No pain associated with the treatment
- All 10 toenails are treated at once (even normal looking nails can have fungal spores hiding in them)
- Shoes and socks can be worn immediately after treatment
- No downtime – each treatment session takes just around 30 minutes
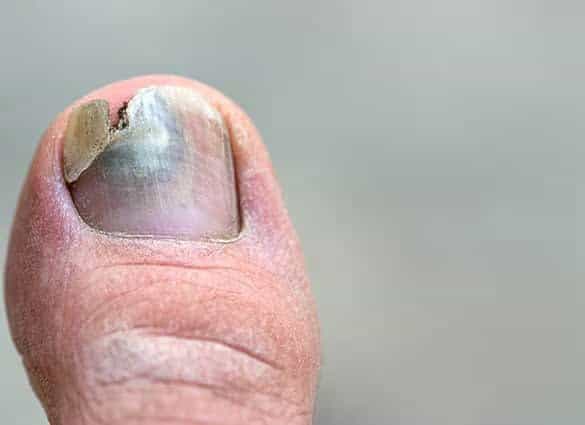
How can I prevent fungal nail infections and reduce recurrence?
You can prevent fungal nail infections and reduce recurrence by:
- Keeping your feet dry throughout the day – wear breathable footwear when possible.
- Wearing socks that wick moisture away from the skin (e.g. Injinji). Change them every day.
- Washing socks / hosiery – in canestan wash and dry them on a hot dryer setting.
- Washing sheets – in canestan wash and dry them on a hot dryer setting.
- Use an antifungal spray or powder (Akileine / Daktarin). Spray or sprinkle your feet and insides of your socks and shoes.
- Apple Cider Vinegar – apply a cotton wool ball soaked in apple cider vinegar for 1 minute to the affected nail.
- Don’t go barefoot in public places. Wear aqua shoes / thongs around public pools, showers, change rooms and campsites.
- Keeping your feet protected in shared bathroom settings. Wear thongs in the bathroom.
- Treating tinea between the toes. If you have tinea between your toes or on your feet, treat it with an antifungal cream.
- Avoiding toe nail polish. Although it may be tempting to hide fungal nail infections under a coat of pretty pink nail polish, this can trap unwanted moisture and worsen the infection.
- Avoiding nail spa pedicures – unless you are sure of strict infection control procedures.
- Nailing care – trim your healthy nails with clean nail clippers and leave your diseased nails for your Podiatrist to attend.
- Avoiding gardening barefoot – avoid submerging your toenails in soil.
- If other member’s of your household have toenail fungus or tinea they will need to be treated to avoid re-infection.
- The dark, moist environment inside of your shoes is the perfect breeding ground for bacteria and fungus, which is believed to re-infect your feet again and again. If you are considering investing in laser treatment for toenail fungus or have already been treated but haven’t completely gotten rid of it we recommend the PediFix ShoeZap Shoe Sanitiser.
What should I do if I have toenail fungus?
Fungal toenails are unsightly, embarrassing, difficult to trim and can spread to your other toenails and fingernails if not treated early.
Our podiatrists in Brisbane Northside can determine the most effective form of treatment for your problem nails, and offer advice on preventive care and the latest in laser therapy to keep your feet healthy and fungus free.