What is Plantar Fasciitis?
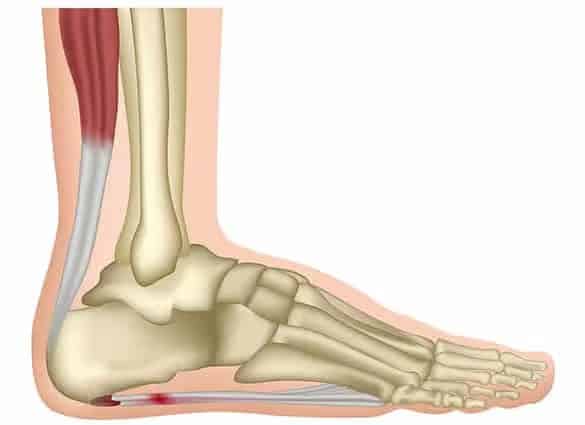
The most common cause of heel and arch pain is a condition called plantar fasciitis. This is an inflammation of a thick band of soft tissue that runs along the arch of your feet from your heel to your toes. The plantar fascia aids in stabilization of your arch during walking and running. Symptoms involve two areas – the arch and, more commonly, the area under your heel bone.
What is the difference between Plantar Fasciitis and Heel Spurs?
Plantar Fasciitis affects the plantar fascia itself, whereas Heel Spurs occur on the heel bone to which the plantar fasciia attaches. Chronic Plantar Fasciitis can lead to the development of Heel Spurs.


What causes Plantar Fasciitis?
Heel and arch pain is usually the result of faulty foot biomechanics and poor foot posture. Abnormal foot function places too much stress on the heel bone and the soft tissues that attach to it. This increased stress causes local inflammation and pain.
Another possible cause is foot muscle weakness. The small intrinsic foot muscles help to support the plantar fascia and stabilise the foot. Weak foot muscles may contribute to increased strain on the plantar fascia.
What factors contribute to the development of Plantar Fasciitis?
Several factors may contribute to the development of plantar fasciitis, all of which place increased strain on the soft tissues beneath your heel:
- Abnormal foot posture – if your feet roll in too much (pronate) the soft tissues beneath your feet become overworked and overstretched causing inflammation and pain.
- Muscle Tightness – Tight calf muscles can result in excessive stress being placed on the plantar fascia.
- Unsupportive footwear with poor shock absorption
- Increased Body Weight
- Increased Activity Levels
- Hard Surfaces – walking on hard surfaces (cement or hard-tiled floors) can aggravate heel pain.


What are the symptoms of Plantar Fasciitis?
Common symptoms of plantar fasciitis include:
- Pain in the morning on the first few steps when you get out of bed
- Pain and stiffness (or hobbling) when you start to walk after sitting for a while
- Increasing pain in your heel towards the end of the day
- A ‘bruised’ feeling or dull ache beneath the heel
- Tired feet and legs by the end of the day
- Pain beneath the heel when walking on hard, unforgiving surfaces (e.g. cement floors or tiles)
How is Plantar Fasciitis diagnosed?
Plantar Fasciitis is usually diagnosed after taking a history and performing a physical examination. The physical examination includes:
- testing your muscle strength
- assessing your joint range of motion and checking for the presence of active trigger points in the foot and leg muscles
- checking your foot posture
- analysing your gait
- testing your ability to perform pain provocation tests
A soft tissue ultrasound of your foot may also be ordered.

Is surgery necessary for Plantar Fasciitis?
There are rare cases of plantar fasciitis that fail to respond to conservative treatment. You should always give conservative treatment at least 6 months to work. If you have a resistant case of plantar fasciitis that fails to respond to conservative treatment a referral to a foot and ankle surgeon may be necessary.
What should I do if I have Plantar Fasciitis?
You should see your podiatrist as soon as possible if you suspect you have plantar fasciitis. The longer heel pain is left untreated, the more difficult it becomes to alleviate with conservative care by your podiatrist. If you think you suffer from or may be at risk of developing plantar fasciitis contact us.


How is Plantar Fasciitis treated?
Plantar fasciitis is the most common complaint of patients of our podiatrists in Brisbane Northside and we find that over 90% of the time, it responds well to our treatment program and surgery is almost never required.
Treatment aims to reduce inflammation of the soft tissues beneath the heel and to improve the alignment and function of your feet. Depending upon the individual contributing factors, treatment may include a combination of the following:
- Rest from aggravating activities and applying ice massage to the heel 3 times daily to reduce inflammation
- Strapping the foot with sports tape can help to reduce excessive strain on the plantar fascia and provide some pain relief
- Custom Made Orthotic inserts for your shoes – to improve your foot posture and reduce strain on the plantar fascia. Research indicates in cases of mechanically induced heel and arch pain, the most effective treatment is quality custom-made foot orthotics. Orthotics are made from a 3-D scan of your feet and are prescribed specifically to help reduce tension on the plantar fascia and to restore normal joint alignment and function.
- Footwear changes – changing to a high quality, stable shoe will help to absorb shock and support and stabilise the foot
- Home Exercise Program – calf muscle and arch stretches are integral to improving foot function and reducing the strain on the plantar fascia
- Joint Mobilisation – in addition to a stretching program, joint mobilizations can help to improve flexibility
- Massage Therapy – can be a helpful adjunct to your treatment
- Dry Needling or acupuncture of trigger points in the muscles of the lower leg and foot can assist in reducing pain and improving muscle function and flexibility
- Medication – in some cases a short course of anti-inflammatory medication may also be required to help reduce acute inflammation
- Weight loss if required
- THOR Low Level Light Laser Therapy
The longer heel pain is left untreated, the more difficult it becomes to alleviate with conservative care by your Podiatrist. If heel pain is not treated early cortisone injections, night stretching splints or cast immobilisation may be required.
Plantar fasciitis sufferers can return to pain-free, full-activity with proper rehabilitation. Return to activity should be gradual and guided by your pain. Proper footwear in combination with corrective orthotics, and a stretching and strengthening program can help prevent reoccurrence of this condition.

