Progressive Arch Collapse
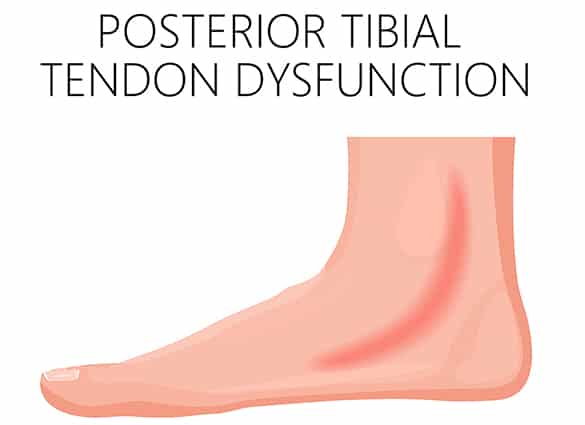
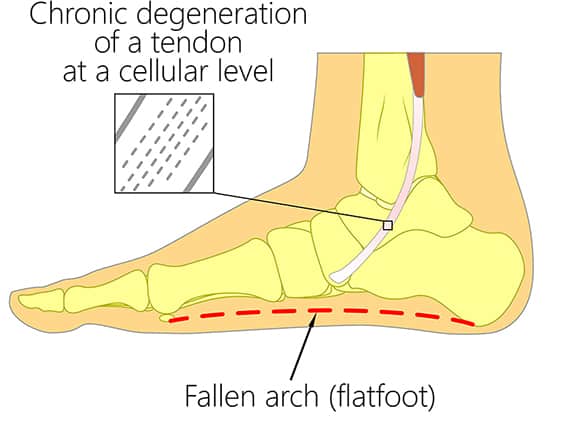
Posterior tibial tendon dysfunction (PTTD) is an injury involving overstretching or rupturing of the posterior tibial tendon, leading to tendon inflammation, weakness, foot deformity and arthritis.
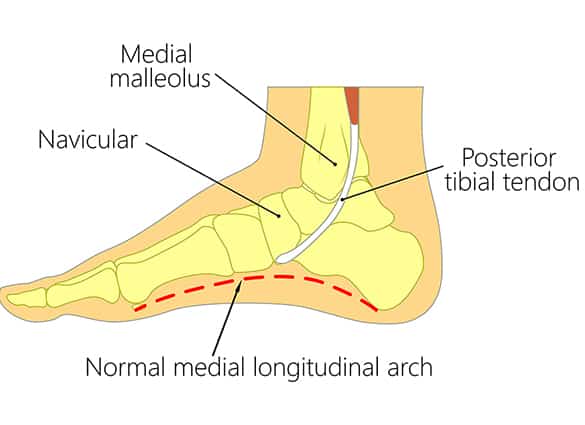
The posterior tibial tendon extends from the deep layer of muscle at the back of your leg. It runs along the inside of your ankle and down the inside of your foot to underneath your arch. This tendon, along with some strong stabilising ligaments, is one of the major supporting structures of the foot.
An important function of the posterior tibial tendon is to help support the arch. In PTTD, the tendon’s ability to perform that job is impaired, often resulting in a collapsed arch or ‘flat foot’. PTTD is the most common type of flat foot developed during adulthood, and is also known as adult-acquired flat foot.
PTTD typically occurs in only one foot, but some people may develop it in both feet. PTTD is usually progressive, meaning it will keep getting worse, especially if it is not treated early.
What are the signs and symptoms of PTTD?
Symptoms of PTTD include:
- pain and swelling on the inside of your ankle, just below or behind the malleolus (ankle bone), which grows worse with increasing activity
- tenderness over the midfoot, especially during activity
- weakness or an inability to stand on your toes
- a collapsed arch and development of a flat foot
- gradually developing pain on the outer side of your ankle
How is PTTD diagnosed?
PTTD is usually diagnosed after taking a history and performing a physical examination. The physical examination includes:
- testing your muscle strength
- assessing your joint range of motion
- checking your foot posture
- analysing your gait
- testing your ability to perform pain provocation tests
A soft tissue ultrasound or plain x-ray of your feet and ankles may also be ordered.
How is PTTD treated?
In most cases, treatment of PTTD begins with non-surgical approaches that may include:
- Immobilisation: your podiatrist may recommend a short removable boot be worn for a few weeks to immobilise your foot and allow your posterior tibial tendon to heal. You will need to avoid all high impact activities (running, jumping, dancing etc) during this period;
- Custom foot orthoses: your podiatrist may recommend a custom-made orthotic device that fits inside your shoe to give your arch the support it needs and help your posterior tibial tendon to rest and heal;
- Footwear: supportive lace-up shoes that provide adequate stability through the arch area and around the heel cup are essential for long term relief from PTTD;
- Physical therapy: a stretching and graduated strengthening exercise program prescribed by your podiatrist may help rehabilitate the posterior tibial muscle and tendon;
- Anti-inflammatory medication: a short course of non-steroidal anti-inflammatory medications (eg. Voltaren, Nurofen) can be a helpful adjunct in reducing inflammation and pain, as can icing the injured tendon;
- Richie Brace: if you require extra support, your podiatrist may recommend a Richie Brace. A Richie Brace is an ankle-foot orthoses that sits inside your shoe, with the brace extending above your ankle.
- Foot Mobilsation Therapy.
When is surgery necessary for PTTD?
In cases of PTTD that have progressed substantially or have failed to improve adequately with non-surgical treatment, surgery may be required. For some advanced cases of PTTD, surgery may be the only option.
Surgical treatment may include repairing the posterior tibial tendon, realigning the bones of the foot, or both. Your podiatrist will refer you to a foot and ankle surgeon who will determine the best approach for your specific case.
What happens if PTTD is left untreated?
Without treatment, the collapsed flat foot that develops from PTTD eventually becomes rigid, and arthritis develops in the foot and ankle. Pain increases and spreads to the outer side of the ankle, and may also appear in the knee and hip. The way you walk may be affected, and finding shoes to fit may become difficult.

How do I know if I am at risk of developing PTTD?
PTTD is most prevalent in women over 50 years of age.
The most common cause of PTTD is overstretching of the posterior tibial tendon.
Symptoms often occur after activities involving the tendon such as walking, running, hiking or climbing stairs.
Other risk factors include:
- obesity
- diabetes
- prior foot surgery or trauma, such as an ankle fracture
- inflammatory diseases such as rheumatoid arthritis and psoriasis
In rare cases, PTTD may also be due to an inherent abnormality of the tendon.
What should I do if I have PTTD?
You should see your podiatrist as soon as possible if you suspect you have PTTD. Because of its progressive nature, early treatment may resolve your symptoms without the need for surgery, and progression of your condition maybe arrested. If left untreated, PTTD could leave you with a flat foot, painful arthritis in your foot or ankle and increasing limitations on walking, running or other activities.
If you think you suffer from or may be at risk of developing posterior tibial tendon dysfunction contact us.